Kafou: Past Present and Future
Kafou, pronounced as written, is the Creole spelling of Carrefour. French words always have a bunch of unpronounced letters and the R’s have to come from down in the throat which is not easy if you are not a native French speaker. Haitian Creole has simplified all that. Kafou/Carrefour is the name of the suburb …
Haiti Update

Thank you all for your thoughts, prayers and concerns for our work and for the country of Haiti. Things have been tense over the past several weeks with violence and protests aimed at overthrowing a corrupt government. Police are in a particularly precarious situation as many of them are in agreement with the aims of …
Manifestations

February 7, 1986 was the day that dictator “baby doc” Duvalier was overthrown in Haiti. To mark this occasion 33 years later and call for the resignation of Haiti’s current president the Haitian people have come out in force. Inflation continues to rise out of control (the gourde is now 82 up from 65 this …
City of Sun

Just 2 months ago Marni and I arrived in Port au Prince. This time it was with one way tickets. This is both literal and figurative. It is not that we won’t be going back to the United States, in fact some voyages are already planned, but we now live in Haiti. We don’t have …
12 Janvier

This is one of those dates that reminds me of where I was at 4:53pm on this same afternoon in 2010. People in America and around the world remember with clarity where we were on the morning of 9-11-2001 when 2996 people lost their lives. Today the Haitians remember every terrifying detail of this same …
Bon Bagay at HAH

Bon Bagay means “Good Stuff” in Kreyol. If you say it a few times it becomes addicting. It is a fitting title for this week’s events. Team Sinai returned for their 7th trip to Hôpital Adventiste d’Haiti. This is a group led by John Herzenberg MD one of the most respected limb deformity surgeons in …
HAH Enters the Digital Age!

As I deplaned at MIA this morning, we were immediately directed towards an escalator leading to the Skytrain. I stepped on to the elevator and the young man about 25 years old right in front of me fell down and dogpiled with the man next to him on top of my bag as I tried …
Dark Side Of Doing Good
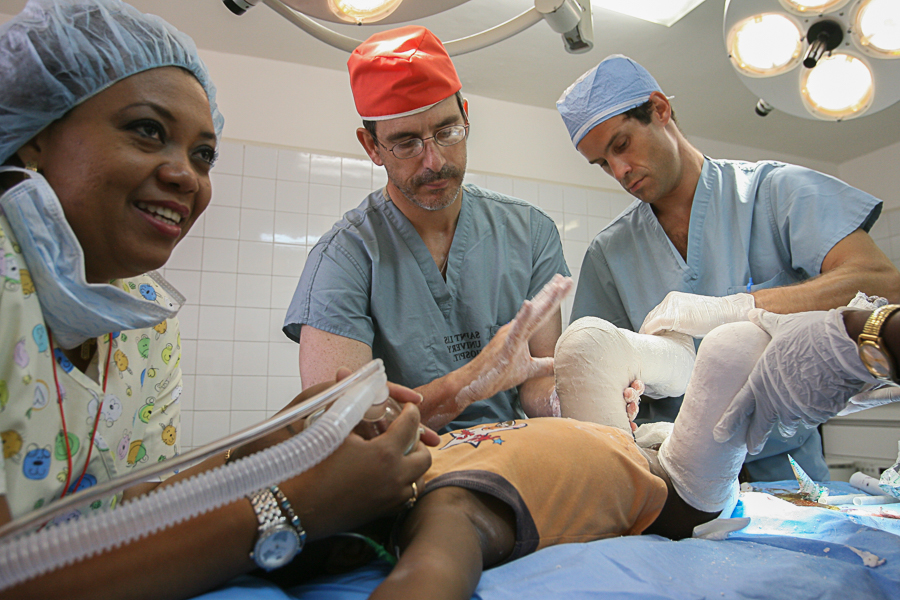
At Loma Linda University’s 2015 Alumni Postgraduate Convention seminar on Global Orthopedics, Merrill Chaus gave both a disturbing and challenging presentation entitled, “The Dark Side Of Doing Good.” Disturbing because, as a veteran of several overseas mission trips, I knew that I had personally violated many of her recommendations – challenging in the sense that …
Recent Comments