Is it possible to be thankful when times are difficult?

David, the great psalmist, says: Enter His gates with thanksgiving and His courts with praise; give thanks to Him and praise His name. For the Lord is good and His love endures forever; His faithfulness continues through all generations. Psalms 100:4-5. It should be easy for us to be thankful when we are comfortable, healthy, …
As gang violence escalates, how is HAH still functioning?
Every day, desperate patients come to Haiti Adventist Hospital (HAH) seeking help not otherwise available. Even if they have a condition potentially treatable in Haiti, they often cannot afford it or may not be able to physically get there due to roadblocks, gang tolls, and disruptions in public transportation. The most respected private hospital in …
Haiti Adventist Hospital Navigates Human-made Disaster

During the past several weeks, the challenges have again escalated beyond imagination. On November 11, the fourth prime minister this year in Haiti was sworn into office. That same day, gunfire penetrated a Spirit Airlines plane on its final approach to Port au Prince airport. Fortunately, no one was seriously injured, and the plane was …
HAH continues to serve in the midst of violence

At the end of February, I packed my carry-on and headed out on a short trip from Haiti back to the US. Several days later, the Haitian airport was commandeered by gangs, and all commercial flights were canceled for three months. Even though it is now possible to fly to Haiti, the situation around the …
What is Happening at HAH?
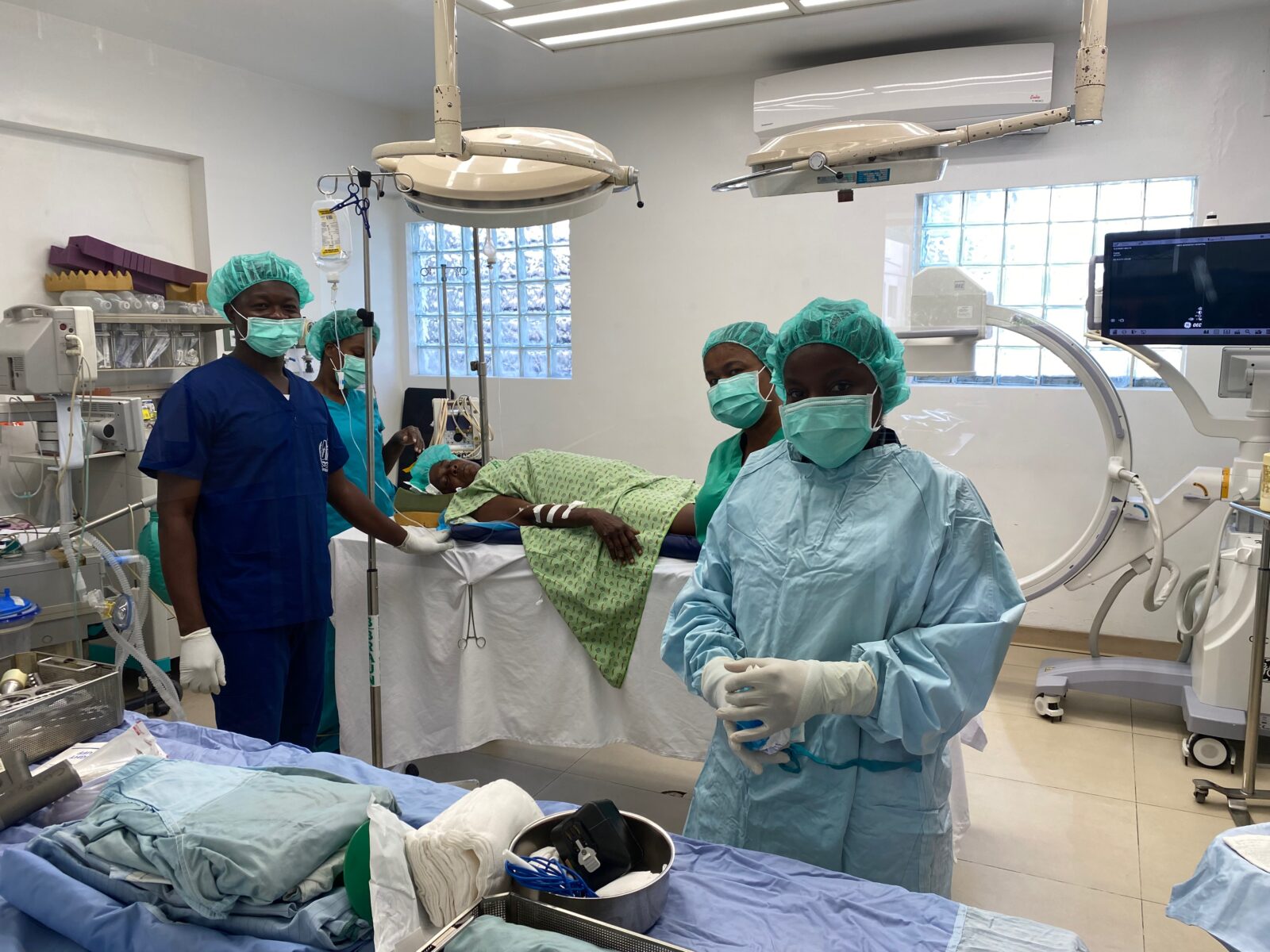
It is no small miracle that Hôpital Adventiste is still functioning given the conflict and challenges around us. Marni and I returned to California in late February for an orthopedic meeting and some work at Loma Linda University. We were planning to return in the beginning of March. Our flights were cancelled the day before …
Man Walks to Church 14 Hours After Operation
At 4:30pm on Friday afternoon, just as I am winding down the workweek, I am notified that we have an open femur fracture in the emergency room. A 37-year-old man was hit by a truck while riding his motorcycle that morning. He originally went to the state hospital ten minutes away, but there is no …
New Clinique Dentaire at HAH
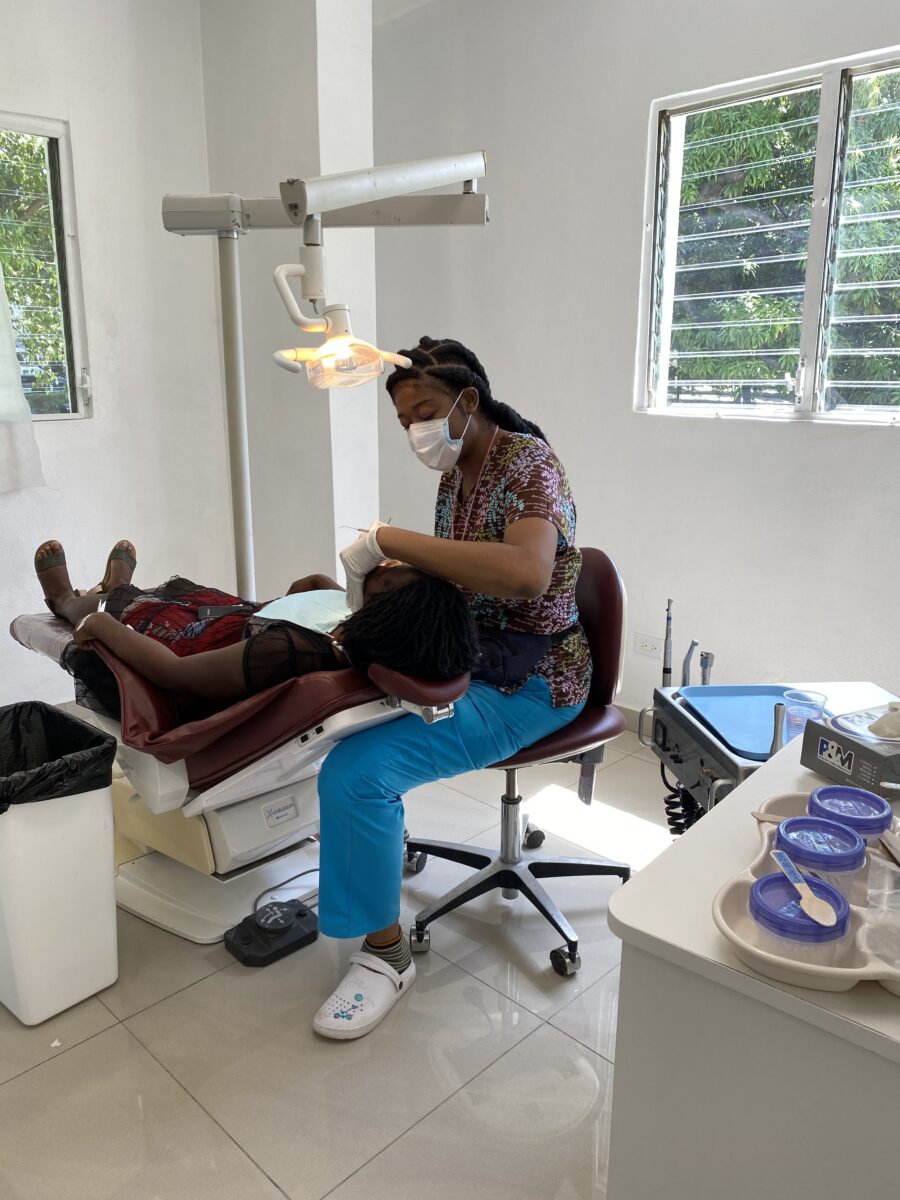
What’s worse, a broken leg or a toothache? A broken leg might be more obvious, but both significantly impact quality of life. HAH has been fixing broken legs for a long time, and now we can also take care of toothaches! Today, three Haitian dentists work in four operatory clinics with several assistants. A new …
Major Renovation Completed at HAH

Six months ago, HAH’s building infrastructure reached a critical turning point. Modifications over the years had affected the natural ventilation of the space, creating dependence on air conditioners that were in a state of disrepair. Patient rooms were stifling hot and humid and smelled of sickness and other bodily odors. Windows were broken, the paint …
Surgeons Finish New Training Program at HAH

The Hôpital Adventiste d’Haiti (HAH) Global Orthopedic Surgery Fellowship recently graduated its first two surgeons, Dr. Conor Spady and Dr. Isaac “Zaco” Archelus. The Global Orthopedic Surgery Fellowship at HAH, endorsed by the Office of Graduate Medical Education at Loma Linda University (LLU), provides experience applying modern surgical techniques to a challenging and unusual variety …
Recent Comments