Global Surgical Need
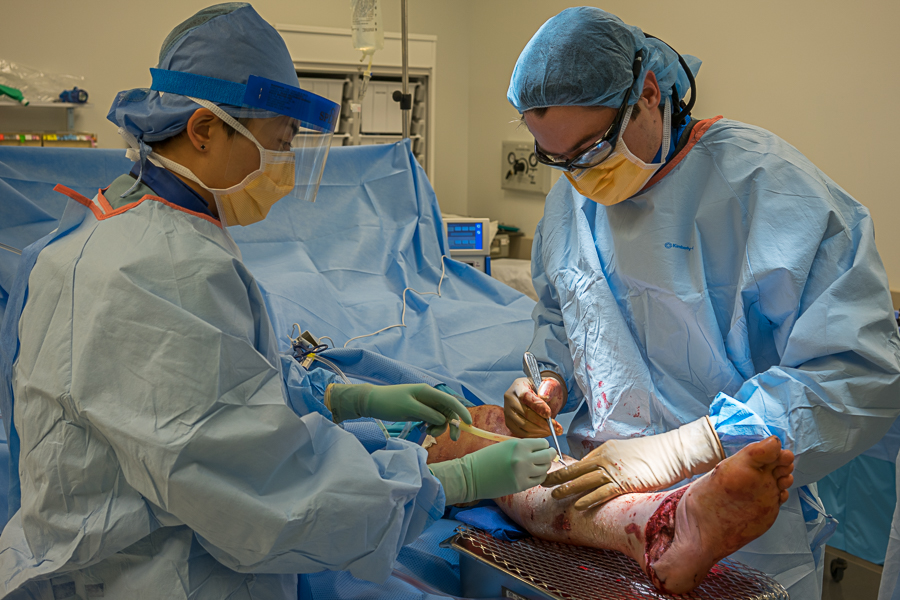
More than 2 billion people are unable to receive surgical care based on operating theatre density alone. The vision of the Lancet Commission on Global Surgery is universal access to safe, affordable surgical and anaesthesia care when needed. The study aimed to estimate the number of individuals worldwide without access to surgical services as defined by …
Almost Ready!

Received a note today from Hopital Adventiste Project Manager Dan Brown stating, “If all goes well we will be moving in on Tuesday, Sept. 29th!” He was referencing, of course, the long-awaited renovation to the new operating theater. To all past and future volunteers and staff, this is great news indeed. The banner image above …
Clean Hands Save Lives

The following article was written by Merrill Chaus, RN and was originally posted on the Team Sinai Haiti blog. Merrill has visited Haiti on numerous occasions and recently wrote an article titled “Dark Side of Doing Good” for haitibones that is well worth reading if you have an interest in volunteering overseas. On August 2, 2015 …
Edward Martin, HAH Administrator

The following update was written by Edward Martin, Administrator of Hopital Adventiste d’Haiti (HAH). Brief Summary The situation under which I was coming to the hospital was less than ideal. In the last quarter of 2013, the hospital ended up losing a very important revenue stream which sent it on a downward spiral. That service accounted …
When “The Good Doctors” Leave
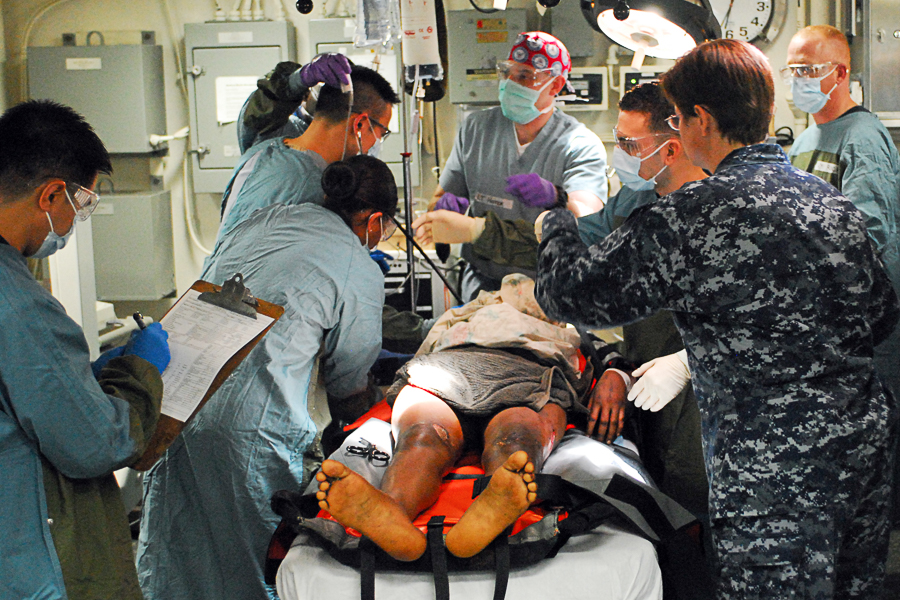
On March 7, 2010 the Los Angles Times published an article written by Joel Rubin entitled “What happens to Haiti when ‘the good doctors’ leave.” The main thrust of Joel’s article was “Emergency medical workers are becoming the de facto healthcare system for a country that has long failed to care for its own. Soon a ragged health …
Dark Side Of Doing Good
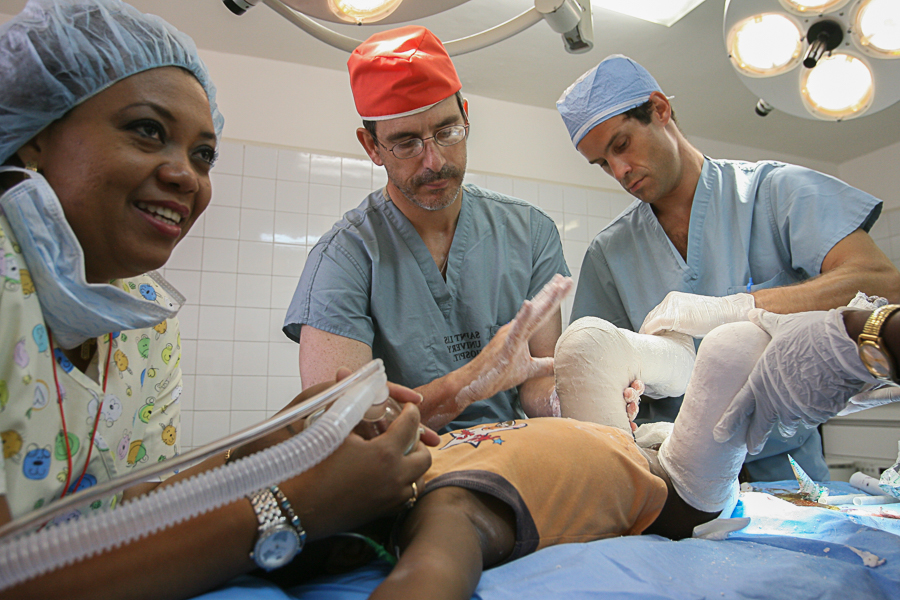
At Loma Linda University’s 2015 Alumni Postgraduate Convention seminar on Global Orthopedics, Merrill Chaus gave both a disturbing and challenging presentation entitled, “The Dark Side Of Doing Good.” Disturbing because, as a veteran of several overseas mission trips, I knew that I had personally violated many of her recommendations – challenging in the sense that …
Matching Gift Opportunity

Florida Hospital announces an exciting matching gift opportunity for Hopital Adventiste d’Haiti (HAH) available now through August 30, 2015. Plans, sketched below, are to renovate the existing polyclinic building and adding outpatient orthopedic services, dental care and optical services. Orthopedic patients at HAH need a location outside of the hospital where follow-up care, consultations and …
Dominik Rog’s Trip To Africa

It is well known that this website is dedicated primarily to the latest news as it relates to Hopital Adventiste d’Haiti (HAH). However from time to time we will feature articles dealing with volunteer experiences outside of Haiti. Dominik Rog is entering his senior year of orthopedic surgery residency at Loma Linda University and has been …
Red Cross In Haiti

This story was reported by Laura Sullivan on behalf of a partnership between NPR News Investigations and ProPublica, an investigative journalism organization. You can read or listen to more of the report on NPR’s site. You can also read more from ProPublica: How the Red Cross Raised Half a Billion Dollars for Haiti and Built …
Haitian Money Pit

After the earthquake in 2010 nearly $10 billion dollars of foreign aid was pledged to rebuild Haiti. Vikram Gandhi went to see just how that money is being put to use. This is his debrief from Season 3, Episode 7 of VICE on HBO. It’s shocking and disappointing to see how little progress the average …
Recent Comments