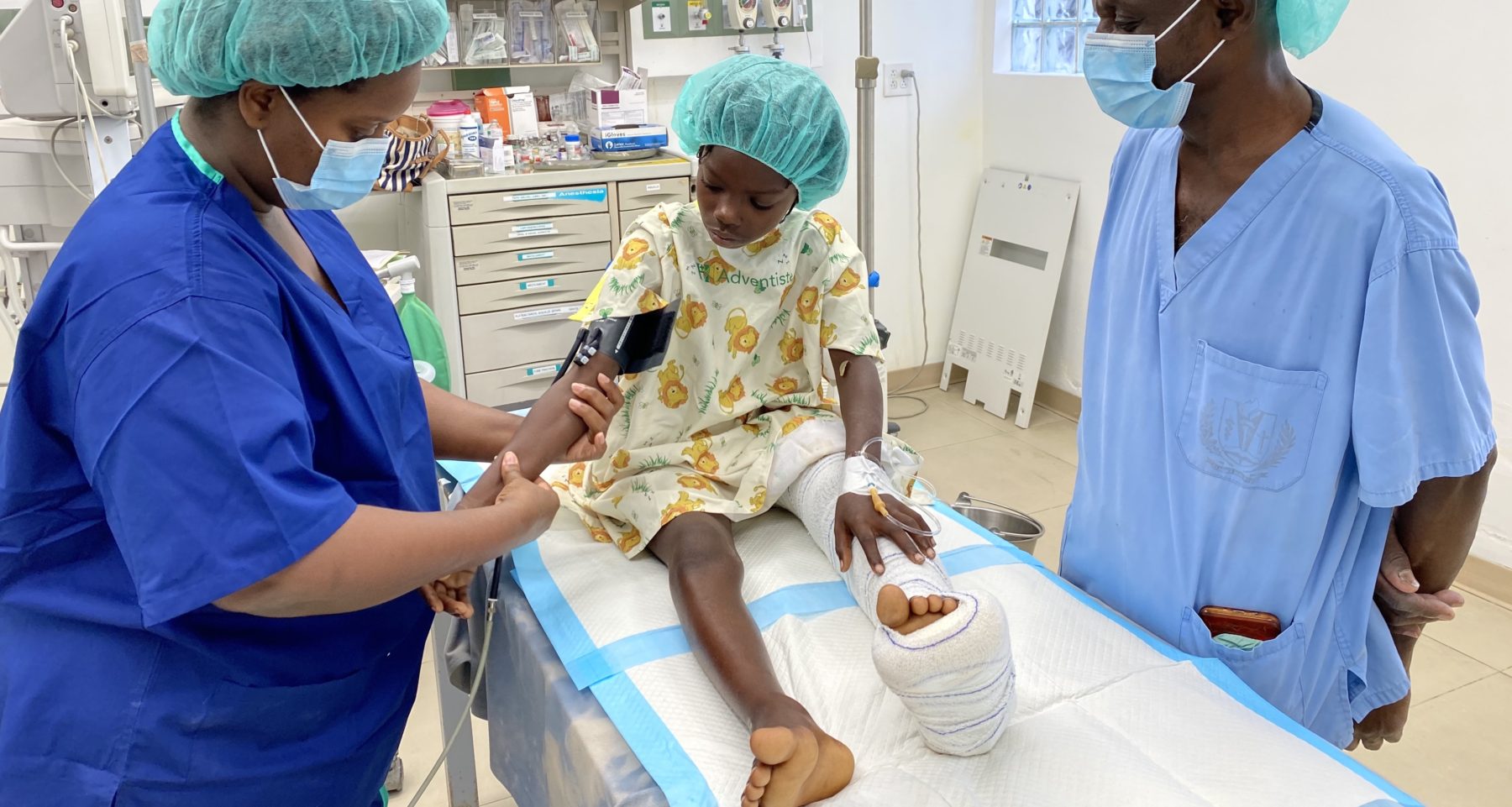
HAH faces another crisis after finishing a record-breaking month of surgical case volume

Before May 2023, our record number of surgeries in a month was 244 cases. That was August 2021 after a major earthquake struck the island, and we worked day and night taking care of major trauma, mostly orthopedic injuries. Since then, our volume has remained high despite being challenged by many crises. Last month we …
Good News from Haiti Adventist Hospital

Though the headlines are not getting any better… It’s like a warzone – Haitians surrounded by turf wars, Gangs gain the upper hand in war with Haitian police, ‘This country is not able to feed itself’: Inside Haiti’s spiralling crisis, Hospitals to close as gangs blockade fuel. In spite of the increasing challenges around us, lots of great stuff …
One month after the earthquake workload at HAH not diminishing

The last few weeks have been a blur. Even before the August 14 earthquake there was rarely a dull moment at HAH. With all the amazing, challenging, and miraculous events taking place, I have been trying to find a few moments of peace in order to share some of the excitement and express gratitude to …
How to Help
We would like to take a “petite pause” to share our heartfelt gratitude with each of you who have reached out to express your love and concern–for the Haitian people, for Hôpital Adventiste d’Haïti, and for each of us. It truly means so much! We regret that we have not been able to reply to …
How HAH is holding up to yet another disaster

Thank you to all who have been reaching out, giving support and thinking and praying for us in Haiti. I will assure all of you that we are just fine and much better off than almost all of those around us. A few missed meals and lost hours of sleep is nothing to worry about. …
What is happening in Haiti that you are not hearing about on the news

In a text message to a friend on Thursday, Rob, a visiting med student sums it up: “Things are insane, but only slightly more than usual”. Sometimes it takes a first time visitor to recalibrate my assessment of a situation. Hôpital Adventiste continues to operate at full capacity. Many challenges remain, but with recent improvements …
Good News at HAH

The Lord is my light and my salvation- whom shall I fear? The Lord is the stronghold of my life- of whom shall I be afraid? When the wicked advance against me to devour me, it is my enemies and my foes who will stumble and fall. Though an army besiege me, my heart will …
HAH is Not on Autopilot

The challenges of working in a foreign country where resources are limited and political strife continues to threaten may never allow us to be on autopilot or operating by remote control. Hôpital Adventiste d’Haiti is a complex machine and we are not on a short or easy journey. Strong headwinds slow us down and at …
Pandemic Update

On the afternoon of March 19 president Jovenal Moise of Haiti in a press conference announced the results of the first positive COVID test in Haiti. At that moment he declared the Port au Prince airport closed and not another commercial passenger airplane has landed since that time. I happened to be on a short …
January 12th

12 January, 2010 I finish a day of work at the Cure Hospital in Santo Domingo, jump on my motorcycle and head out for the evening commute. This involves winding in between gridlocked vehicles jumping the curb a few times and finding any small path to make the 2 mile commute a little more efficient. …
Recent Comments