Dominik Rog’s Trip To Africa

It is well known that this website is dedicated primarily to the latest news as it relates to Hopital Adventiste d’Haiti (HAH). However from time to time we will feature articles dealing with volunteer experiences outside of Haiti. Dominik Rog is entering his senior year of orthopedic surgery residency at Loma Linda University and has been …
Red Cross In Haiti

This story was reported by Laura Sullivan on behalf of a partnership between NPR News Investigations and ProPublica, an investigative journalism organization. You can read or listen to more of the report on NPR’s site. You can also read more from ProPublica: How the Red Cross Raised Half a Billion Dollars for Haiti and Built …
Haitian Money Pit

After the earthquake in 2010 nearly $10 billion dollars of foreign aid was pledged to rebuild Haiti. Vikram Gandhi went to see just how that money is being put to use. This is his debrief from Season 3, Episode 7 of VICE on HBO. It’s shocking and disappointing to see how little progress the average …
“I’d Rather Have HIV Than A Broken Leg”
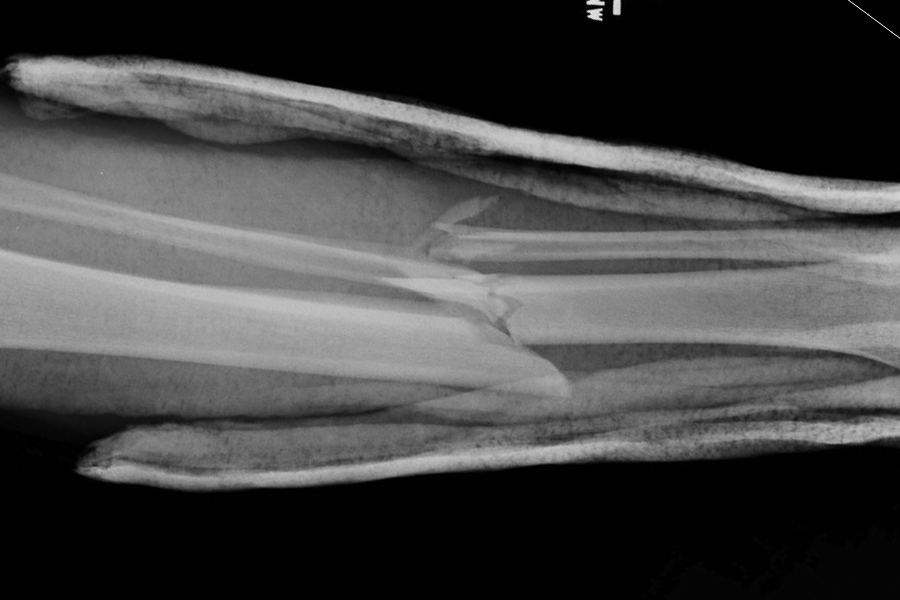
The video below was filmed at an independently organized TEDx event and features Edward O’Bryan, an emergency room physician from South Carolina and cofounder of the Palmetto Medical Initiative. His monologue serves as a poignant reminder that trauma, particularly the musculoskeletal variety, remains a neglected epidemic in developing countries, causing more than five million deaths each year, …
Thank-you To Our Nepali Friends

The tenth installment of the May, 2015 Loma Linda University Health Orthopedic Team visit to Nepal. All of our team members made it safely back to California several days ago, in fact Elaine Lewis is already back to work in Haiti. All in all, it was an amazing trip one that we will long remember. Since …
Tales Of Loss And Survival

Click here to get a brief view of the staggering human toll in Nepal, and just like many of the souls in Haiti after their earthquake tragedy, you will get a glimpse of the resiliency of those who survived. Scheer Memorial Hospital continues to treat victims of both the April 25 and May 12 earthquakes that crippled …
New Life In The Midst Of Tragedy

The ninth installment of the May, 2015 Loma Linda University Health Orthopedic Team visit to Nepal was written by surgical technician Elaine Lewis. In addition to her duties in the operating room, Elaine has many years experience as a midwife back home in California and was able to participate in the birth of two lives shortly …
Namaste Nepal

Part 8 of the May, 2015 Loma Linda University Health Orthopedic Team visit to Nepal. In addition to the April 25 7.8 magnitude quake, the devastated Nepali people were dealt another blow in the form of a 7.3 magnitude trembler on May 12. Please consider donating to Adventist Health International’s Nepal Earthquake Fund as there is still …
Fear On Assignment

Part 7 of the May, 2015 Loma Linda University Health Orthopedic Team visit to Nepal. The following post was written by Andrew Haglund, logisitical supporter for our team. Andrew’s eyewitness account was also posted on CNN’s iReport. (This and subsequent updates from Nepal will be intermittent and delayed due to marginal internet access at SMH). The …
Shakedown In The OR
Part 6 of our May, 2015 Loma Linda University Health Orthopedic Team visit to Nepal. A new earthquake of 7.3-magnitude hit devastated Nepal on May 12, just 17 days after large parts of Nepal were leveled and more than 8,000 had died. The following post was written by Dr Scott Nelson who was operating at …
Recent Comments