Man Walks to Church 14 Hours After Operation
At 4:30pm on Friday afternoon, just as I am winding down the workweek, I am notified that we have an open femur fracture in the emergency room. A 37-year-old man was hit by a truck while riding his motorcycle that morning. He originally went to the state hospital ten minutes away, but there is no …
New Clinique Dentaire at HAH
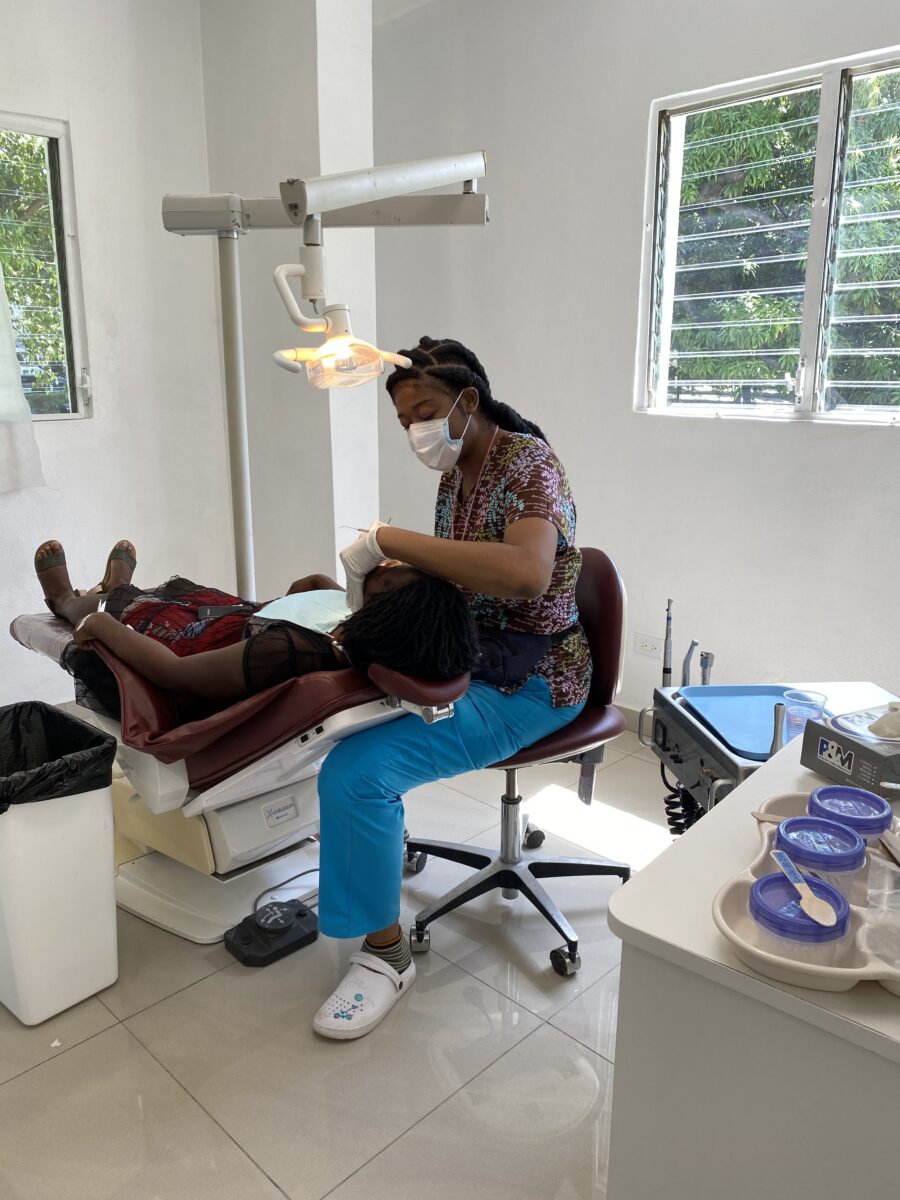
What’s worse, a broken leg or a toothache? A broken leg might be more obvious, but both significantly impact quality of life. HAH has been fixing broken legs for a long time, and now we can also take care of toothaches! Today, three Haitian dentists work in four operatory clinics with several assistants. A new …
Major Renovation Completed at HAH

Six months ago, HAH’s building infrastructure reached a critical turning point. Modifications over the years had affected the natural ventilation of the space, creating dependence on air conditioners that were in a state of disrepair. Patient rooms were stifling hot and humid and smelled of sickness and other bodily odors. Windows were broken, the paint …
Surgeons Finish New Training Program at HAH

The Hôpital Adventiste d’Haiti (HAH) Global Orthopedic Surgery Fellowship recently graduated its first two surgeons, Dr. Conor Spady and Dr. Isaac “Zaco” Archelus. The Global Orthopedic Surgery Fellowship at HAH, endorsed by the Office of Graduate Medical Education at Loma Linda University (LLU), provides experience applying modern surgical techniques to a challenging and unusual variety …
HAH faces another crisis after finishing a record-breaking month of surgical case volume

Before May 2023, our record number of surgeries in a month was 244 cases. That was August 2021 after a major earthquake struck the island, and we worked day and night taking care of major trauma, mostly orthopedic injuries. Since then, our volume has remained high despite being challenged by many crises. Last month we …
Good News from Haiti Adventist Hospital

Though the headlines are not getting any better… It’s like a warzone – Haitians surrounded by turf wars, Gangs gain the upper hand in war with Haitian police, ‘This country is not able to feed itself’: Inside Haiti’s spiralling crisis, Hospitals to close as gangs blockade fuel. In spite of the increasing challenges around us, lots of great stuff …
One month after the earthquake workload at HAH not diminishing

The last few weeks have been a blur. Even before the August 14 earthquake there was rarely a dull moment at HAH. With all the amazing, challenging, and miraculous events taking place, I have been trying to find a few moments of peace in order to share some of the excitement and express gratitude to …
How to Help
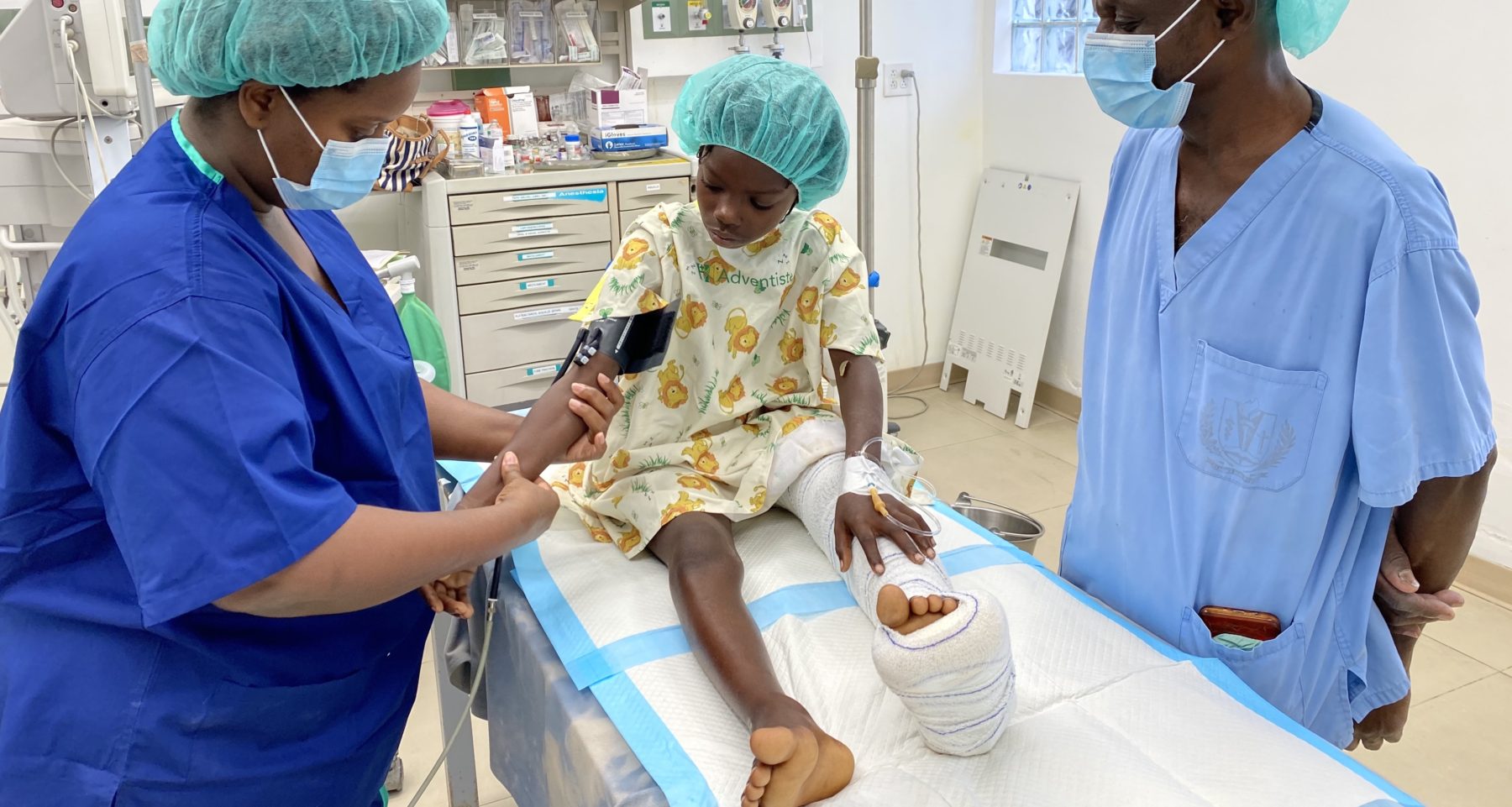
We would like to take a “petite pause” to share our heartfelt gratitude with each of you who have reached out to express your love and concern–for the Haitian people, for Hôpital Adventiste d’Haïti, and for each of us. It truly means so much! We regret that we have not been able to reply to …
How HAH is holding up to yet another disaster

Thank you to all who have been reaching out, giving support and thinking and praying for us in Haiti. I will assure all of you that we are just fine and much better off than almost all of those around us. A few missed meals and lost hours of sleep is nothing to worry about. …
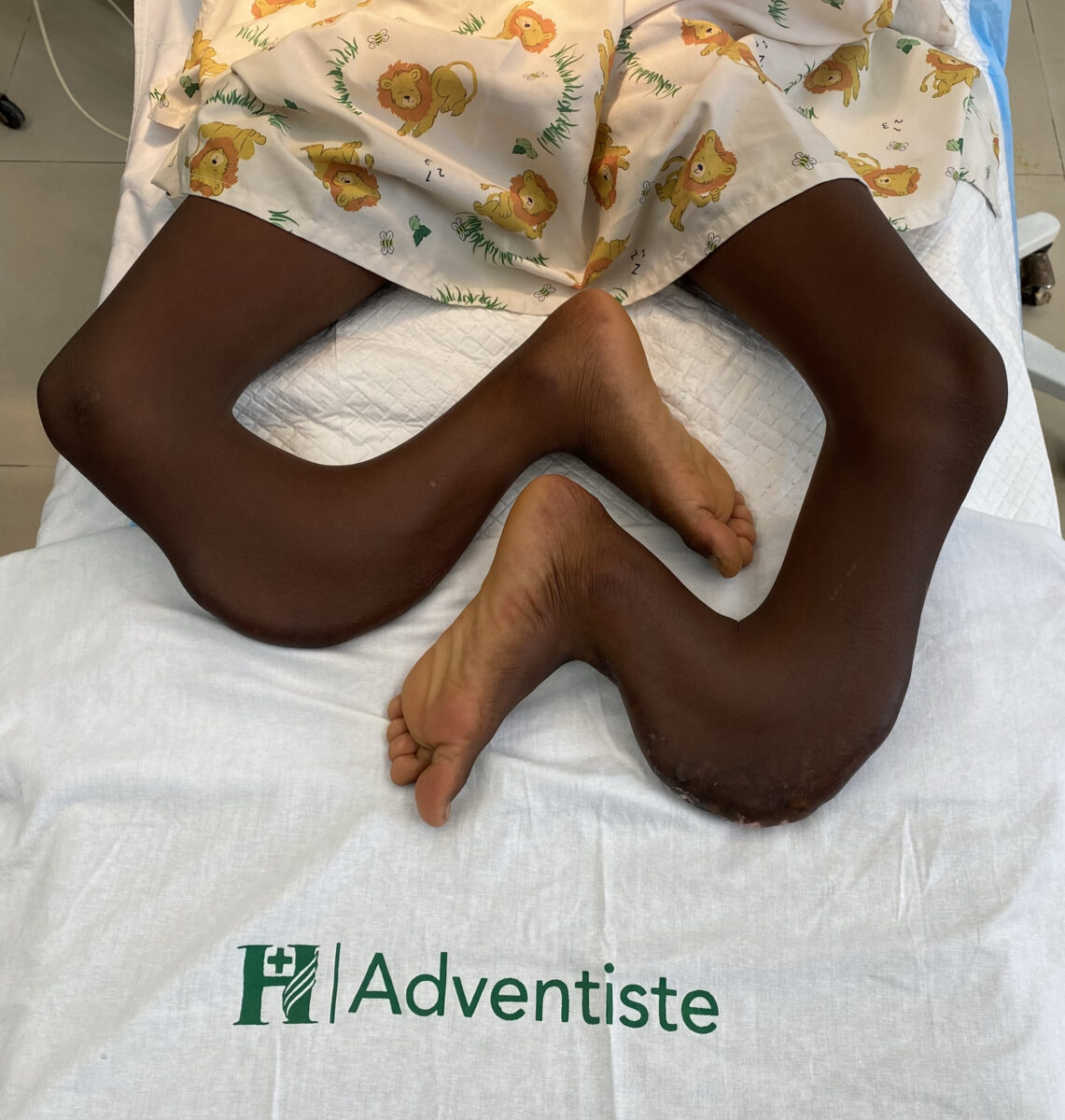
Recent Comments